Autism spectrum disorder (ASD) is known for challenges in social interaction, communication, and behavior. However, many people don’t realize that unusual brain electrical activity – EEG spikes – often co-occurs with autism. Studies show that anywhere from about 24% up to 60% of children with ASD have epileptiform activity (electrical “spikes” or seizure-like discharges) on an electroencephalogram (EEG), even if they’ve never had a noticeable seizure[1]. In some cases, these hidden EEG spikes can worsen developmental problems or even mimic autism symptoms. Intriguingly, there are reports that treating these abnormal brain spikes with the right medication has dramatically improved children’s symptoms – even to the point that some children no longer met the criteria for autism. In this post, we’ll explore what EEG spikes are, how they can manifest like autism, and which medical treatments have helped children improve.
EEG Spikes That Can “Look Like” Autism
Figure: EEG recording from a 5-year-old autistic child during sleep, showing frequent spike-wave discharges (blue peaks) in the brain’s right posterior region[2]. Such continuous spike-wave activity (often seen in epileptic encephalopathy like ESES) can disrupt language and behavior.
EEG “spikes” are abnormal bursts of electrical activity in the brain. They are often seen in epilepsy, but they can also occur without visible seizures – these are called subclinical epileptiform discharges. Research has found that children with autism frequently have these EEG abnormalities: one review noted interictal epileptic discharges (spikes between seizures) in 20% of autistic children during awake EEG, and over 40% during sleep EEG[3]. Importantly, these brain spikes can affect development. For example, in a condition called Electrical Status Epilepticus in Sleep (ESES), children have almost continuous spikes during deep sleep. This leads to a regression or loss of skills – especially language – that can closely resemble autism. In fact, the deterioration of language and behavior in ESES can range from “severe global deterioration compatible with the diagnosis of disintegrative disorder or ASD” (essentially an autism-like state) to milder learning problems[4]. A classic case is Landau-Kleffner Syndrome (LKS), where a child (often around age 3–7) suddenly loses language skills due to epileptic EEG spikes in the language centers. Such a child may appear autistic (becoming nonverbal and socially withdrawn) until the true cause is recognized. These examples show that excessive EEG spiking can produce autism-like symptoms, blurring the line between an “autism” diagnosis and an underlying electrical brain disorder.
Researchers are still unraveling how EEG spikes tie into autism. One theory is that persistent spikes disrupt the forming brain networks, especially during critical periods of development. The spikes may interfere with sleep-dependent brain processes (like memory consolidation and language acquisition) and lead to autistic behaviors. Interestingly, spikes are more common in autistic children who have regression (loss of skills) or intellectual disability[5][6]. It’s even been suggested that autism with early seizures or regression might be a special subtype of ASD[7]. All this raises a hopeful question: if these EEG spikes contribute to autistic symptoms, could treating the spikes improve those symptoms? In the next section, we look at several cases where doctors tried exactly that – and saw promising results.
Medication That Tamed the Spikes – and Transformed Kids’ Lives
For many years, the conventional wisdom was skeptical that you should treat EEG spikes if the child wasn’t having obvious seizures. A prominent neurologist, Dr. Isabelle Rapin, once wrote that there was “little evidence to suggest that seizure-free children with rare spikes or other paroxysmal EEG discharges will benefit from anticonvulsants”[8]. In other words, why medicate if the spikes aren’t causing visible seizures? However, recent research and case studies have challenged this view, showing that in some children, suppressing those hidden spikes can lead to remarkable developmental gains.
Valproic Acid (VPA): One striking example comes from a report by Dr. Audrius Plioplys in the 1990s. He treated three young autistic children (ages 3, 4, and 5) who had epileptiform EEG spikes but no outward seizures, using a low dose of the anti-seizure medication valproic acid. Within one month, all three children showed such improvement in language and social interaction that they no longer met the DSM criteria for autism[9]. In other words, after valproate suppressed their brain spikes, their autism symptoms lessened to the point that the diagnosis effectively “went away.” This dramatic change was sustained at follow-ups 7–11 months later[9]. Such cases suggest that some children diagnosed with ASD might have been primarily affected by an underlying electrical disturbance – treat the disturbance, and the “autism” symptoms recede. It’s important to note this is a small sample, but it provided proof-of-concept that medication can make a life-changing difference for certain kids.
Corticosteroids (Prednisolone/ACTH): Another line of evidence comes from treating autistic regression as an inflammatory or epileptic phenomenon. Steroids – powerful anti-inflammatory drugs – are a standard treatment for epileptic regression syndromes like LKS or infantile spasms. Neurologists began trying them in children with regressive autism (children who had developed typically but then lost skills around age 1–2). In one retrospective study at Boston Children’s Hospital, 20 young children with regressive autism received steroid therapy (prednisolone) and were compared to similar kids who didn’t get steroids. The steroid-treated group showed significant clinical improvement in their language (both understanding and speaking) and in autistic behaviors after treatment[10]. In fact, improvements were seen on an objective brain-wave measure tied to language (the FMAER evoked potential), suggesting the steroids calmed whatever brain dysfunction was present[10]. Almost all the treated kids had some side effects (steroids can cause weight gain, high blood pressure, mood changes, etc.), but these were mostly mild or reversible[10]. This study[11] provides encouraging evidence that even if a child meets autism criteria, medical therapy aimed at brain inflammation or epileptic activity can improve core symptoms. Similarly, another case report documented a child with autism symptoms and an autoimmune disorder who received low-dose steroids; the child’s speech and developmental milestones significantly improved following treatment[12]. Parents of previously non-verbal children have reported sudden language gains after such treatments – for example, a toddler who had lost all words began speaking again after steroid therapy in these reports. These are isolated cases, but they offer hope that some “non-verbal autism” might be partly reversible when the right medical trigger is addressed.
A related therapy is adrenocorticotropic hormone (ACTH), a hormone therapy often used for difficult epilepsy. A 2017 study looked at 25 patients with ASD or ADHD plus severe stuttering, all of whom had ESES (the nighttime spike barrage we described earlier). They treated them with ACTH and achieved full normalization of their EEGs. Amazingly, along with the EEG improvement came a 72% average improvement in the children’s autism/ADHD symptoms (as measured by clinical scales)[13]. Several kids’ stuttering resolved completely as well. The researchers noted a clear correlation: the more the spike activity (spike-wave index) went down, the more the child’s behavior and attention improved[13]. This hormone treatment, while not routine for autism, again underscores the principle – calm the abnormal brain activity, and the child’s developmental trajectory can change. In practical terms, some children who were profoundly affected (non-verbal, severe behaviors) became much more communicative and engaged after these treatments. One mother whose child underwent steroid/AED therapy described it as “waking up” her child from a fog.
Other Antiepileptic Drugs (AEDs): Aside from valproate, doctors have explored other seizure medications in ASD with EEG spikes. Levetiracetam (Keppra), for instance, has shown mixed but intriguing results. A small placebo-controlled trial in children with autistic regression and spikes found levetiracetam significantly reduced the spike discharges[14]. The children’s cognitive testing hinted that when spikes were higher, verbal learning was worse, implying spikes were holding them back[15]. However, in that short trial the overall behavioral improvements didn’t reach significance on a group level[16] – some kids improved, others not much. Clinicians have also reported using ethosuximide (for absence-like spike-wave discharges) or benzodiazepines at bedtime (to suppress nocturnal spikes) in autistic children, especially those with sleep-activated discharges. For example, children with autistic regression due to ESES often receive benzodiazepines or high-dose diazepam during sleep, sometimes leading to dramatic improvements in language. While controlled studies are scarce, about 70% of children in one series who had developmental delays and epileptiform EEGs showed definite improvement after starting an antiepileptic drug[17]. This was observed within one clinic visit (i.e. relatively soon after treatment)[17]. Such findings give weight to the idea that clinicians should at least consider an EEG and perhaps a medication trial when an autistic child’s development seems unusually stalled or regressed.
What This Means for Parents and Researchers
The stories above sound almost miraculous – an autistic child speaks for the first time after medication, or loses their diagnosis after treatment. It’s important to understand that these cases represent a subset, not the majority, of autism situations. Autism is a very diverse condition, and most children with ASD do not suddenly become non-autistic from a course of pills. However, this emerging research is extremely valuable because it highlights a previously underappreciated factor: in some children, autistic symptoms are exacerbated by underlying brain electrical disturbances that can be treated. For parents, especially those of children who experienced a regression or who have abnormal EEG results, it is empowering to know that medical evaluation could open new avenues. If your autistic child has periods of staring, night wakings, unexplained regressions, or other hints of seizure-like activity, bringing this up with a neurologist and getting an EEG might be worthwhile. As one expert noted, even though the “yield” of finding treatable EEG issues in autism is not fully known, if an intervention can prevent or ameliorate a life-long disorder, even a low yield is justified[18]. In plain terms: finding nothing on an EEG causes little harm, but if you find something and can treat it, you might change the child’s life.
For researchers and clinicians, these findings open up exciting and challenging questions. We need to better identify which children with ASD have an “electrical” component to their symptoms – possibly through overnight EEGs or even advanced scans like MEG (magnetoencephalography). Interestingly, one study using MEG found spikes in 82% of autistic patients, while standard EEG detected them in only 68%[19], suggesting we might be under-detecting brain spikes with routine methods. Another question is when to treat and what to treat with. Small studies like the ones cited give us hints: valproate, steroids, ACTH, and levetiracetam each helped in certain scenarios[9][10][13]. But we need larger, controlled trials to know which children will respond and to ensure safety. Steroids, for example, have significant side effects, so their use must be carefully weighed against the benefits[20][21]. The good news is that the medical community is taking this seriously: there are clinical trials and ongoing research into “treatable autisms”, recognizing that what looks like primary autism in some children might actually be secondary to an underlying neurological condition (like subclinical epilepsy or neuroinflammation). Early evidence already indicates that suppressing interictal discharges can improve behavior in children, even if they don’t have full epileptic seizures[17].
EEG spikes can sometimes masquerade as autism or significantly worsen an existing autism condition. For a subset of children, treating those spikes with the appropriate medication (whether an anticonvulsant or anti-inflammatory therapy) has led to meaningful improvements – improvements in communication, behavior, and overall development. A few have even lost their autism diagnosis after treatment[9], showing just how profound the impact can be. This doesn’t imply a “cure” for all autism, but it does offer a ray of hope that identifying and addressing co-occurring neurological issues can help some children reach their full potential. For parents, the takeaway is to be vigilant and open-minded about medical evaluations; for professionals, it’s to continue researching and personalizing treatments for autism. The line between neurology and psychiatry is thinner than ever in ASD, and by looking at the brain’s electrical activity, we just might unlock new ways to help our kids. As science advances, what we learn from these EEG spikes might not only improve individual lives but also deepen our understanding of the diverse biology underlying “autism” itself.
Harnessing AI to Uncover Effective Autism Treatments
In the first part of this article, we discussed patterns such as spikes (e.g. epileptiform EEG spikes) observed in some autistic children, and how identifying these patterns can guide treatment decisions. Now in this part, we focus on how advanced AI—especially large language models (LLMs) like GPT—can help recognize which medications have led to significant improvements in autistic children. Specifically, we explore how AI can sift through past studies and clinical data to pinpoint treatments that reduced autism symptoms to the point that some children no longer meet the diagnostic criteria. We also provide a table of various medications and their observed effects on children with autism, based on evidence from research.
AI and LLMs for Identifying Promising Autism Medications
Treating autism spectrum disorder (ASD) is challenging because no medication currently cures ASD, and existing drugs only target specific symptoms[1][2]. Two antipsychotic medications (risperidone and aripiprazole) are FDA-approved to manage irritability, aggression and repetitive behaviors in autistic children[3]. However, these only address associated behavioral problems and do not improve core social-communication deficits of autism[2]. Each autistic individual can respond differently to medications, so finding an effective drug often involves trial-and-error[1]. This is where artificial intelligence can play a transformative role.
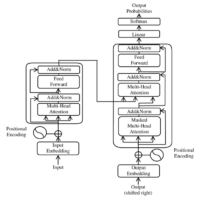
Large Language Models (LLMs) like GPT can analyze vast amounts of text-based information—including medical literature, clinical trial results, and even electronic health records—to detect patterns and insights far beyond the capacity of a human clinician. AI systems can be trained to comb through physician notes, research papers, and patient histories to discover, for example, that a subset of children with specific neurological patterns responded extremely well to a particular treatment. In fact, researchers are already developing AI models that suggest personalized treatments for ASD by integrating complex datasets (genetic data, lab results, diagnoses) with the unstructured information in doctors’ written notes[4]. By processing natural-language observations from physicians about what did or didn’t help each patient, an AI can learn which interventions led to meaningful improvements[4]. This means an LLM-based system could read through decades of autism case reports and clinical studies to find hidden connections—for instance, linking EEG spike patterns with responsiveness to certain anti-seizure medications.
Pattern recognition in text: An AI could identify all mentions in literature where “after treatment X, autism symptoms significantly improved” or “child no longer met ASD criteria.” For example, prior studies note that treating subclinical epileptic “spikes” in autistic children with anticonvulsants like valproic acid can yield dramatic improvements[5]. An AI could quickly gather all such cases, helping researchers compile a list of medications that have led to the greatest reductions in autism symptoms. The AI might flag small trial results, case series, or even parent reports that humans might overlook individually. By aggregating this knowledge, LLMs can generate hypotheses about which medications (or combination of treatments) are most worth investigating for broader use.
Below, we summarize some medications and treatments that have shown notable positive effects in some children with ASD. This illustrates the kind of information AI can extract from past research to guide future autism therapy.
Medications with Notable Effects in Autism (Examples)
The table below highlights several medications that studies or trials have associated with significant improvements in autistic children. In some instances, children’s symptoms improved so much that they no longer met the diagnostic criteria for ASD or showed major gains in functioning. These examples underscore how mining previous studies (a task well-suited to AI) can identify promising treatments. All listed effects are supported by research findings:
| Medication (Mechanism) | Observed Effects in Autistic Children |
| Valproic Acid (anticonvulsant) | In ASD children with epileptiform EEG spikes but no obvious seizures, low-dose valproate led to striking improvements. Within 1 month of VPA (125 mg thrice daily), language and social skills improved, and the children no longer met DSM criteria for autism[5]. This suggests some autism-like behaviors were driven by subclinical brain electrical disturbances that valproate helped normalize. |
| Levetiracetam (anticonvulsant) | A randomized trial in autistic children with subclinical seizures found that adding levetiracetam (Keppra) for 6 months improved their outcomes. Levetiracetam controlled EEG discharges and was associated with improved cognitive and behavioral function compared to controls[6]. This supports treating “spikes” in ASD, as reducing these abnormal brain activities can improve attention, learning and behavior. |
| Bumetanide (diuretic; GABA modulator) | Multiple trials of bumetanide (a diuretic that affects the brain’s GABA signaling) show it can alleviate core autism symptoms. In one trial, 3 months of low-dose bumetanide yielded a significant reduction in autism severity scores (CARS) and improved clinical global impressions compared to no treatment[7]. Bumetanide is thought to rebalance the excitatory/inhibitory signals in the brain, and about one-third of treated children showed notable improvement in social communication and reduced repetitive behaviors. |
| Suramin (antipurinergic experimental drug) | A small placebo-controlled trial at UC San Diego tested a single IV dose of suramin in boys with ASD. All five treated boys showed measurable improvements in language, social interaction, and restricted behaviors within weeks[8]. Autism diagnostic scores (ADOS-2) improved by an average of 1.6 points with suramin (no change in placebo), and if a child’s score drops to 6 or below, they “no longer meet the formal diagnostic criteria for ASD”[9]. The improvements were transient (lasting ~5–6 weeks), but parents reported unprecedented gains – for instance, one 14-year-old nonverbal boy began speaking in sentences and “advanced almost three years in development in just six weeks” after suramin[10]. |
| Folinic Acid (Leucovorin, a vitamin B9 analog) | Some autistic children have metabolic or folate-related abnormalities. A placebo-controlled trial of high-dose folinic acid (2 mg/kg per day) for 12 weeks found significantly improved verbal communication in the treated group[11]. Language scores rose ~5.7 points (medium-large effect size) versus placebo, with the greatest gains seen in children who had folate receptor autoantibodies[12]. Parents and clinicians also noted improvements in adaptive behavior and social responsiveness in the folinic acid group[13]. This suggests that addressing underlying nutritional/biochemical issues can reduce some autism symptoms. |
| Risperidone & Aripiprazole (atypical antipsychotics) | These medications reduce severe irritability, aggression, and self-injurious outbursts in autistic children[3]. By calming challenging behaviors and decreasing tantrums, they can improve a child’s ability to participate in learning and social activities. However, they do not target core communication or social deficits of ASD[2], and they carry notable side effects (weight gain, sedation, etc.). Thus, they are used for symptom management rather than as autism “cures.” |
Table: Examples of medications/treatments and their effects on ASD symptoms, as reported in studies. Some interventions (like valproate, levetiracetam, bumetanide, suramin, and folinic acid) address underlying neurological or metabolic factors and have led to notable improvements in certain children. Others (like antipsychotics) manage externalizing behaviors. This is not an exhaustive list; rather, it illustrates the range of biomedical treatments that AI could analyze when searching for effective autism therapies.
How AI Can Synthesize Past Research for Autism Treatment
Given the diversity of findings in autism research, AI tools are invaluable for connecting the dots. A large language model can rapidly read and synthesize thousands of research papers and clinical reports. For instance, it can extract data on which medications helped which subgroup of patients (e.g. kids with epilepsy-like EEG patterns, kids with specific genetic syndromes, or those with GI issues). By comparing outcomes, an AI might detect that treating co-occurring conditions (like epilepsy, gut microbiome imbalance, or immune dysfunction) often leads to significant autism symptom improvement. Indeed, clinicians have noted that identifying and treating such comorbidities can yield “optimal outcomes” in some ASD cases[14].
LLMs like GPT could be used to generate literature reviews or evidence maps on autism interventions. For example, an AI could list all trials where an experimental drug (such as suramin or bumetanide) was tested, summarize the results, and even highlight methodological strengths/weaknesses of each study. This helps researchers and doctors stay up-to-date on rapidly evolving findings. Rather than manually reading hundreds of papers, a clinician could ask an AI: “What medications have been reported to significantly improve social functioning in autism?” and receive an aggregated answer with references (much like the table above, but distilled from the entire body of literature).
Moreover, precision medicine for autism can be enhanced by AI. Autism is extremely heterogeneous—what works for one child may not work for another[15]. AI algorithms can learn from individual patient data to predict responses. For example, the precision medicine model being developed by Iyer and colleagues uses AI to propose treatments based on complex factors like a patient’s genetics, lab results, and past responses[16]. Crucially, that system also parses doctors’ written observations to judge how well a medication helped or what side effects occurred[4]. This is essentially an application of natural language processing (the technology underpinning LLMs) to real-world data. It shows how GPT-style AI can read free-text medical notes and extract clinically useful insights, such as “Child A’s aggression dropped when on medication X, but language did not improve” – information that might otherwise remain buried in one child’s chart.
Mining patient records: In large healthcare systems, there may be hundreds of autistic patients’ records. An AI could be deployed to read all these (de-identified) records to find patterns – say, children with high inflammation markers responded to immunotherapy, or those with frequent EEG spikes benefited from valproate. Such findings can then be systematically studied. This approach, often called retrospective data mining or real-world evidence analysis, is greatly accelerated by LLMs that understand clinical language.
Generating new hypotheses: Beyond summarizing known results, AI can help generate hypotheses for new treatments. For instance, by analyzing biomedical texts, an LLM might notice parallels between autism and another condition at the molecular level, suggesting a drug used for that other condition could be repurposed for ASD. (This is how bumetanide, a blood-pressure diuretic, was identified – researchers hypothesized it could correct a neurotransmitter imbalance in autism[17][2].)
Towards AI-Guided Autism Therapy Discoveries
In summary, AI and LLMs stand to greatly accelerate the discovery of effective autism treatments by collating the collective knowledge from past studies and patient experiences. They can rapidly recognize which medications have yielded significant improvements (“spikes” of success) and under what circumstances. As we saw, there are already documented cases where children’s autism symptoms markedly lessened after certain medical interventions[5][9]. The challenge is that these cases are scattered across different studies and medical records.
By using advanced natural language processing, we can connect these valuable dots. In practice, this means an AI could recommend, for example: “Consider an EEG for this non-verbal child; if epileptic spikes are present, anti-seizure medication might dramatically improve speech” – an insight drawn from prior cases like the valproate study. Or for a child with ASD and gastrointestinal problems, AI might highlight research on microbiota transfer or folinic acid, pointing to potential improvements in behavior[18][11].
It’s important to note that AI is a tool to assist, not replace, clinical judgment. Any AI-flagged treatment would still require validation through clinical trials or careful patient-specific evaluation. Ethical use of LLMs in healthcare also demands ensuring data privacy and avoiding biases. That said, the ability of AI to learn from the past at scale offers hope for more pinpointed, effective interventions going forward. Researchers are already calling this approach “precision medicine for ASD”, where treatments are tailored to an individual’s unique profile, aided by AI analysis[19][20].
In conclusion, leveraging LLMs and AI can help the autism community make sense of vast and complex data – revealing which medications and therapies have truly made a difference. By systematically identifying the factors that helped some children essentially outgrow their autistic features, AI could guide us toward new breakthroughs, turning anecdotal successes into broadly applicable treatments. The ultimate vision is that with AI’s help, future autistic children might receive more personalized, effective care – potentially minimizing debilitating symptoms and improving their quality of life to the fullest extent possible.
[1] [4] [15] [16] [19] [20] Precision medicine model uses AI to target ASD | Health Care Engineering Systems Center | Illinois
https://healtheng.illinois.edu/news/60712
[2] [7] [17] Symptom improvement in children with autism spectrum disorder following bumetanide administration is associated with decreased GABA/glutamate ratios | Translational Psychiatry
[3] New advances in the diagnosis and treatment of autism spectrum disorders | European Journal of Medical Research | Full Text
https://eurjmedres.biomedcentral.com/articles/10.1186/s40001-024-01916-2
[5] Abnormal EEG in Autism: Valproate Response | Pediatric Neurology Briefs
https://pediatricneurologybriefs.com/articles/10.15844/pedneurbriefs-8-3-7
[6] Levetiracetam is associated with decrease in subclinical epileptiform discharges and improved cognitive functions in pediatric patients with autism spectrum disorder – PubMed
https://pubmed.ncbi.nlm.nih.gov/28919764
[8] [9] [10] Century-old drug could provide new approach to autism | University of California
https://www.universityofcalifornia.edu/news/century-old-drug-could-provide-new-approach-autism
[11] [12] [13] [14] Folinic acid improves verbal communication in children with autism and language impairment: a randomized double-blind placebo-controlled trial – PubMed
https://pubmed.ncbi.nlm.nih.gov/27752075
[18] Autism symptoms reduced nearly 50% 2 years after fecal transplant | ASU News
Recent research and case reports on ASD with epileptiform EEG abnormalities and treatments[1][9][17][10][13].
[1] [3] [5] [6] [7] Frontiers | Electroencephalography in Assessment of Autism Spectrum Disorders: A Review
https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2021.686021/full
[2] Continuous Spike–Waves during Slow Sleep Today: An Update
https://www.mdpi.com/2227-9067/11/2/169
[4] [14] [15] [16] [17] [18] [19] EEG changes associated with autistic spectrum disorders | Neuropsychiatric Electrophysiology | Full Text
https://npepjournal.biomedcentral.com/articles/10.1186/s40810-014-0001-5
[8] Autism: Electroencephalogram Abnormalities and Clinical Improvement With Valproic Acid | JAMA Pediatrics | JAMA Network
https://jamanetwork.com/journals/jamapediatrics/article-abstract/517039
[9] Abnormal EEG in Autism: Valproate Response | Pediatric Neurology Briefs
https://pediatricneurologybriefs.com/articles/10.15844/pedneurbriefs-8-3-7
[10] [11] [12] [20] [21] Corticosteroid therapy in regressive autism: Preliminary findings from a retrospective study | BMC Medicine | Full Text
https://bmcmedicine.biomedcentral.com/articles/10.1186/1741-7015-12-79
[13] ACTH reduces autism & stuttering
https://www.thinkingautism.org.uk/acth-therapy-benefits-stuttering-and-autism